In modern clinical diagnostics, even the smallest technical detail can influence a patient’s diagnosis. One such detail—often overlooked outside laboratory environments—is the Blood-to-Anticoagulant Ratio in EDTA Tubes. This ratio plays a decisive role in maintaining blood sample integrity, ensuring reliable test results, and preventing costly diagnostic errors.
EDTA tubes are widely used for hematology tests such as the Complete Blood Count (CBC), coagulation screening, and blood banking procedures. While most healthcare professionals are familiar with EDTA as an anticoagulant, fewer fully appreciate how sensitive blood analysis is to the correct blood-to-anticoagulant balance.
This in-depth guide explains why the Blood-to-Anticoagulant Ratio in EDTA Tubes is a critical factor, how it affects laboratory results, what happens when the ratio is incorrect, and how to ensure optimal performance using high-quality EDTA tubes from trusted manufacturers like EDTATube.
To understand EDTA tubes themselves, you can start with this detailed overview from EDTATube’s main resource hub, which explains tube types, uses, and standards in clinical settings.
EDTA Tubes and Their Role in Blood Collection
EDTA, or ethylenediaminetetraacetic acid, is a chelating agent that prevents blood clotting by binding calcium ions. Since calcium is essential for the coagulation cascade, removing it ensures that blood remains fluid during storage and testing.
In routine laboratory practice, EDTA tubes are used for hematology tests because they preserve cellular morphology better than many other anticoagulants. Red blood cells, white blood cells, and platelets maintain their size and shape when the Blood-to-Anticoagulant Ratio in EDTA Tubes is correct.
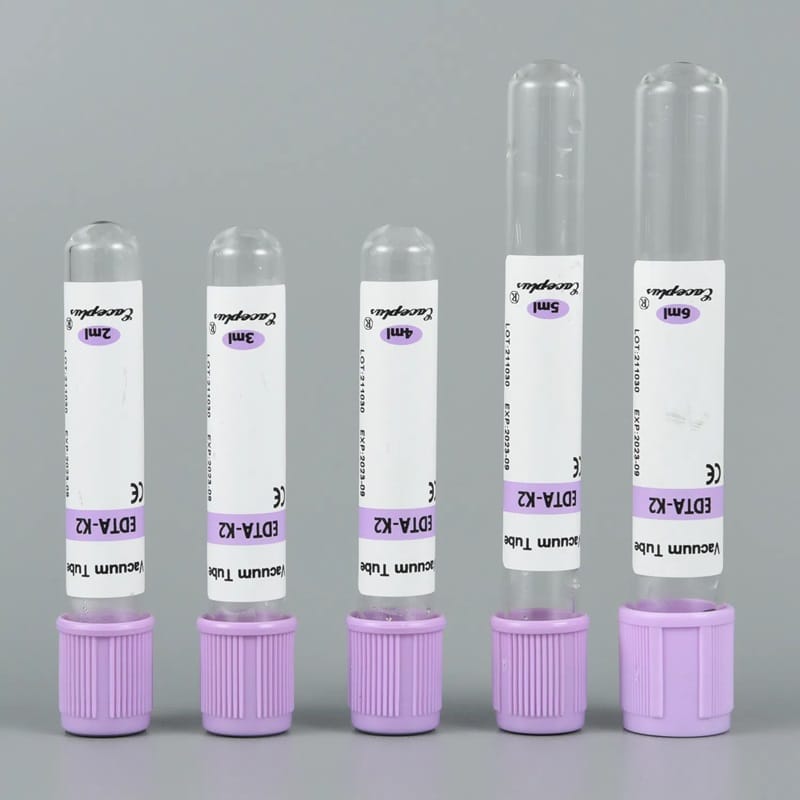
Manufacturers design EDTA tubes with precisely calculated anticoagulant volumes based on the intended blood draw capacity. For example, a 3 mL EDTA tube contains a different EDTA concentration than a 10 mL tube. These calibrated ratios are critical for maintaining sample accuracy.
You can explore various tube capacities and specifications in the EDTA tube product category to see how manufacturers match anticoagulant dosage with tube volume.
Why the Blood-to-Anticoagulant Ratio in EDTA Tubes Matters
The Blood-to-Anticoagulant Ratio in EDTA Tubes directly influences test accuracy. Laboratories rely on this balance to ensure that blood cells remain unchanged from the moment of collection to analysis.
When the ratio is correct, EDTA prevents clotting without damaging blood cells. However, when the ratio is altered—either by underfilling or overfilling the tube—test results can become unreliable.
For hematology tests such as the Complete Blood Count, even small distortions in cell size or platelet count can lead to incorrect diagnoses. Conditions like anemia, thrombocytopenia, or leukocytosis may be misinterpreted due to improper anticoagulant ratios.
This is why international standards emphasize correct tube filling as strongly as proper sample labeling or storage temperature.
What Happens When EDTA Tubes Are Underfilled
Underfilling is one of the most common errors affecting the Blood-to-Anticoagulant Ratio in EDTA Tubes. When too little blood enters the tube, the EDTA concentration becomes excessive relative to blood volume.
Excess EDTA can cause red blood cells to shrink, leading to falsely low mean corpuscular volume (MCV) values. Platelets may swell or fragment, resulting in inaccurate platelet counts. In some cases, EDTA toxicity may even cause cell membrane damage.
These distortions are particularly problematic in pediatric or emergency settings where small blood volumes are common. Laboratories may need to reject samples entirely, leading to delays in patient care.
Using appropriately sized tubes, such as 3 mL or 4 mL EDTA vacuum tubes, significantly reduces underfilling risks.
Risks Associated with Overfilling EDTA Tubes
Overfilling EDTA tubes can be just as problematic. When too much blood is added, the EDTA may be insufficient to fully chelate calcium ions. An incorrect Blood-to-Anticoagulant Ratio in EDTA Tubes caused by overfilling may result in partial clot formation. These microclots often go unnoticed until laboratory analysis, where they interfere with automated analyzers. Clotted or partially clotted samples compromise white blood cell differentials and platelet counts. Laboratories often discard these samples, requiring repeat collections and increasing patient discomfort.
Standard Blood-to-Anticoagulant Ratios Explained
Most EDTA tubes are manufactured to maintain a ratio of approximately 1.5–2.2 mg of EDTA per mL of blood, depending on whether K2 or K3 EDTA is used. K2 EDTA is spray-dried on the tube walls and is widely preferred for hematology testing because it causes minimal dilution. K3 EDTA is liquid-based and slightly dilutes the sample, making accurate filling even more critical.A deeper explanation of EDTA chemistry can be found in this technical guide on EDTA anticoagulant principles.
Impact on Hematology and Blood Banking Applications
The Blood-to-Anticoagulant Ratio in EDTA Tubes is especially important in blood banking. EDTA preserves antigen integrity on red blood cells, which is essential for blood typing, crossmatching, and antibody screening. Inaccurate ratios can affect agglutination reactions, potentially leading to mismatched transfusions. That is why blood banks rely heavily on standardized EDTA tubes for sample consistency. To learn more about this application, refer to blood banking with EDTA tubes, which outlines best practices and safety considerations.
Choosing High-Quality EDTA Tubes for Accurate Ratios
Not all EDTA tubes are manufactured to the same standard. High-quality tubes ensure uniform anticoagulant coating, precise vacuum pressure, and consistent internal volume. Manufacturers like EDTATube follow strict quality control processes to maintain the correct Blood-to-Anticoagulant Ratio in EDTA Tubes across every batch. You can explore certified options such as disposable medical consumable EDTA blood collection tubes designed for laboratory accuracy and safety.
Storage, Handling, and Mixing Techniques
Even the best tube cannot compensate for improper handling. After collection, EDTA tubes should be gently inverted 8–10 times to mix blood with the anticoagulant. Vigorous shaking damages cells, while insufficient mixing creates localized clotting. Both scenarios disrupt the Blood-to-Anticoagulant Ratio in EDTA Tubes and compromise results. Proper disposal is also critical for safety and compliance. Guidance on disposal procedures can be found in this authoritative resource on disposing blood collection tubes.
Regulatory Standards and Global Guidelines
International bodies such as CLSI and ISO emphasize standardized blood collection procedures. These guidelines reinforce the importance of correct filling volumes and validated EDTA tube designs. Educational resources like this complete guide to EDTA tubes provide additional insights into compliance and best practices.
The Role of EDTA Plasma Separator Tubes
Some laboratories use EDTA plasma separator tubes for specialized testing. These tubes include gel barriers and require even stricter control of the Blood-to-Anticoagulant Ratio in EDTA Tubes. A technical overview is available in this complete guide on EDTA plasma separator tubes, which explains their design and applications.
Summary
Blood-to-Anticoagulant Ratio in EDTA Tubes is not a minor technical detail—it is a cornerstone of accurate laboratory diagnostics. From hematology to blood banking, this ratio determines whether test results reflect true patient conditions or misleading artifacts.By using high-quality EDTA tubes, following proper collection techniques, and respecting manufacturer guidelines, healthcare professionals can protect sample integrity and patient safety. Trusted suppliers like edta tube play a vital role in supporting reliable diagnostics worldwide. For product inquiries or technical support, visit edta tube and contact us.
FAQs
Why is the Blood-to-Anticoagulant Ratio in EDTA Tubes so important?
The Blood-to-Anticoagulant Ratio in EDTA Tubes ensures accurate blood cell preservation, preventing false results in hematology and blood banking tests.
Can incorrect filling affect CBC results?
Yes, an incorrect Blood-to-Anticoagulant Ratio in EDTA Tubes can alter cell size, platelet counts, and white blood cell morphology, leading to inaccurate CBC results.
Which EDTA type is better, K2 or K3?
Both work effectively, but K2 EDTA is often preferred because it causes less dilution, helping maintain the correct Blood-to-Anticoagulant Ratio in EDTA Tubes.
How can laboratories prevent ratio errors?
Using properly sized tubes, following fill guidelines, and sourcing tubes from reliable suppliers help maintain the Blood-to-Anticoagulant Ratio in EDTA Tubes.
Do storage conditions affect the ratio?
Improper storage can degrade EDTA effectiveness, indirectly impacting the Blood-to-Anticoagulant Ratio in EDTA Tubes during analysis.